Introduction
Asthma is a long-term disease of the lungs. Asthma is a condition in which airways narrow and swell and may produce extra mucus. Asthma is a serious disease that affects about 25 million Americans and causes nearly 2 million emergency room visits every year. With treatment, the patient can live well. Without it, might have to go to the ER often or stay at the hospital, which can affect daily life.
Definition
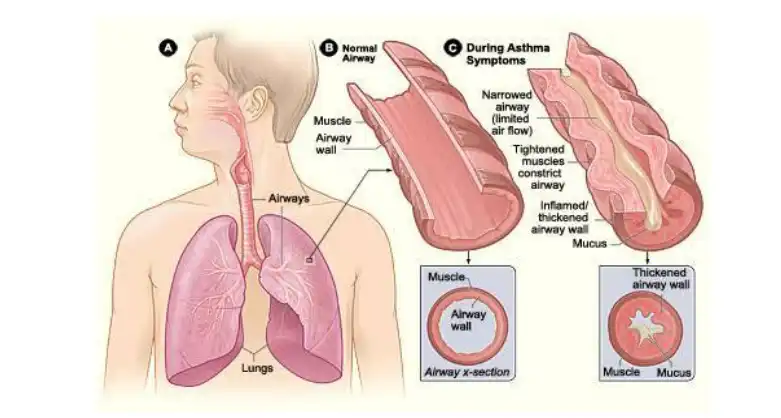
Asthma is a lung disease that inflames and narrows our airways. Normally, when inhale, air moves freely through the trachea, or windpipe, then through large tubes, called bronchi, smaller tubes, called the bronchioles, and finally into tiny sacs, called alveoli.
Types of Asthma
• Adult-Onset Asthma.
• Allergic Asthma.
• Asthma-COPD Overlap.
• Exercise-Induced Bronchoconstriction (EIB)
• Nonallergic Asthma.
• Occupational Asthma
The root cause of asthma
Various irritants and substances that trigger allergies (allergens) can trigger signs and symptoms of asthma. Asthma triggers are different from person to person and can include: Airborne allergens, such as pollen, dust mites, mold spores, pet dander or particles of cockroach waste.
Signs and symptoms
-Wheezing
-Cough
-Shortness of breath
-Tachycardia
-Difficulty breathing
-Pale and wet skin
-Dyspnea
-Chest tightness
Causes
Asthma causes are different from person to person and can include:
• Airborne allergens, such as pollen, dust mites, mold spores, pet dander, or particles of cockroach waste.
• Respiratory infections, such as the common cold
• Physical activity
• Cold air, air pollutants, and irritants, such as smoke
• Certain medications, including beta-blockers, aspirin, and nonsteroidal anti-inflammatory drugs, such as ibuprofen (Advil, Motrin IB, others) and naproxen sodium (Aleve)
• Strong emotions and stress
• Sulfites and preservatives added to some types of foods and beverages, including shrimp, dried fruit, processed potatoes,
beer and wine
• Gastroesophageal reflux disease (GERD), a condition in which stomach acids back up into your throat
Complications
Asthma complications include:
• Signs and symptoms that interfere with sleep, work, and other activities
• Sick days from work or school during asthma flare-ups
• A permanent narrowing of the tubes that carry air to and from your lungs (bronchial tubes), which affects how well you can
breathe
• Emergency room visits and hospitalizations for severe asthma attacks
• Side effects from long-term use of some medications used to stabilize severely asthma Proper treatment makes a big difference in preventing both short-term and long-term complications caused by asthma.
Risk factors
Some factors are thought to increase the chances of developing asthma. They include:
• Having a blood relative with asthma, such as a parent or sibling
• Having another allergic condition, such as atopic dermatitis — which causes red, itchy skin — or hay fever — which causes a
runny nose, congestion, and itchy eyes
• Being overweight
• Being a smoker, exposure to secondhand smoke
• Exposure to exhaust fumes or other types of pollution
• Exposure to occupational triggers, such as chemicals used in farming, hairdressing, and manufacturing
Foods To Avoid With Asthma
Foods rarely trigger an asthma attack. But the symptoms of a severe allergic reaction to some foods can mimic asthma symptoms. The first step is to know if you have a food allergy. Any abnormal reaction to food is considered an adverse reaction.
• Food allergy: When your immune system reacts to proteins in foods that usually are safe or harmless. Your doctor can do skin tests to find out if you’re sensitive to certain foods.
• Food intolerance: When your body responds to the food, not your immune system. Examples include food poisoning, reactions to chemicals in food or drinks such as caffeine, or reflux. The most common foods associated with allergic symptoms are:
• Eggs
• Cow’s milk
• Peanuts
• Soy
• Wheat
• Fish
• Shrimp and other shellfish
• Tree nuts
Food Preservatives and Asthma Food preservatives can also trigger an asthma attack. Additives, such as sodium bisulfite, potassium bisulfite, sodium metabisulfite, potassium metabisulfite, and sodium sulfite, are commonly used in food processing or preparation and can be found in foods such as:
• Dried fruits or vegetables
• Potatoes (packaged and some prepared)
• Wine and beer
• Bottled lime or lemon juice
• Shrimp (fresh, frozen, or prepared)
• Pickled foods
Symptoms of Food Allergies and Asthma
For most people, the usual symptoms of food allergies are hives, rash, nausea, vomiting, and diarrhea. If you have food allergies that trigger symptoms of an asthma attack, will likely have these allergy symptoms, followed by coughing and wheezing. And if not caught quickly, anaphylaxis swelling of the throat, cutting off airway may result.
Prevention
While there’s no way to prevent asthma, the doctor can design a step-by-step plan for living with a patient’s condition and preventing asthma attacks.
• Asthma action plan. Asthma is an ongoing condition that needs regular monitoring and treatment. Taking control of treatment can make patients feel more in control of life.
• Get vaccinated for influenza and pneumonia. Staying current with
vaccinations can prevent flu and pneumonia from triggering asthma flareups.
• Identify and avoid asthma triggers. A number of outdoor allergens and irritants — ranging from pollen and mold to cold air and air pollution — can trigger asthma attacks. Find out what causes or worsens asthma, and take steps to avoid those triggers.
• Monitor your breathing. You may learn to recognize warning signs of an impending attack, such as slight coughing, wheezing or shortness of breath. But because your lung function may decrease before you notice any signs or symptoms, regularly measure and record your peak airflow with a home peak flow meter. A peak flow meter measures how hard you can breathe out. Your doctor can show you how to monitor your peak flow at home.
• Take your medication as prescribed. Don’t change your medications without first talking to your doctor, even if your asthma seems to be improving. It’s a good idea to bring your medications with you to each doctor visit. Your doctor can make sure you’re using your medications correctly and taking the right dose.
• Pay attention to increasing quick-relief inhaler use. If you find yourself relying on your quick-relief inhaler, such as albuterol, your asthma isn’t under control. See your doctor about adjusting your treatment.
Conclusion –
Asthma is an important chronic disease resulting in clinically significant morbidity, missed days of work or school, substantial costs for emergency care and hospitalization, and sometimes, death. Current therapy can control asthma and may prevent the development of irreversible airway changes in asthmatic patients.